From the article you will learn what to do with varicose veins in the legs, how to relieve swelling, features of conservative and surgical therapy, and preventive measures.
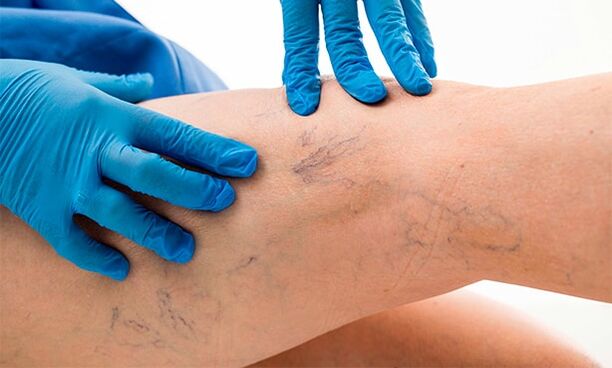
Varicose veins are a chronic venous pathology, which is based on a malfunction of the valve apparatus, causing stagnation of blood flow with dilation and inflammation of blood vessels, and an increase in tissue pastiness.
General information
The initial manifestations are the formation of spider veins, swelling of the saphenous veins, the formation of nodes, painful veins, and heaviness in the legs.As the disease progresses, signs of chronic venous circulation insufficiency appear: swelling of the feet and legs, cramps in the calf muscles, trophic ulcers, thrombophlebitis, ruptures of varicose veins.According to various studies in the field of clinical phlebology, varicose veins affect 30 to 40% of women and 10 to 20% of men over the age of 18 years.
Usually, when talking about varicose veins, they mean an independent disease - varicose veins of the lower extremities.Varicose veins are manifested by a feeling of heaviness in the legs and their fatigue, swelling of the feet and legs, night cramps in the legs, visual subcutaneous dilation of the veins with the formation of venous nodes.
Why do veins dilate?
To understand this issue, you need to imagine how the blood, which has successfully supplied oxygen to the body tissues, returns back to the heart.To overcome the force of gravity, rising from the legs to the chest, it needs auxiliary mechanisms.First of all, we are talking about the muscles of the lower extremities, which act as a pump: their contraction during walking moves blood to the heart.In addition, valves located inside the veins play an important role in this process: they prevent the reverse flow of blood.
Varicose veins are a disease of valves that have ceased to perform their function.As a result of this disorder, fluid accumulates in the vessels, which leads to their expansion.
In the future, trophic ulcers may develop in the area of deformed veins, and blood clots formed due to blood stagnation contribute to the occurrence of a severe and deadly complication of varicose veins - pulmonary embolism.
Varicose veins of the legs are common among women and men - signs of pathology are observed in more than half of people over 18 years of age.At the same time, the number of patients is growing every year - this is due to the sedentary nature of professional activity.
Often, varicose veins of the lower extremities are accompanied by another well-known disease - hemorrhoids.The nature of occurrence of both diseases is the same, as are the risk factors predisposing to their development.As in the case of varicose veins, people often ignore the symptoms of hemorrhoids until the last moment, hoping that the pathology will go away on its own.However, these diseases are irreversible without radical intervention and only progress over time.
It is believed that the main causes of varicose veins are: congenital weakness of connective tissue, hormonal changes, prolonged forced sitting or standing.Long legs and tall stature are a risk factor for varicose veins.When a person stands, the valves in the veins are open.The higher the column of blood in the vessels, the higher the pressure.Excess weight also increases pressure in the veins of the legs - fat deposits, especially in the abdominal area, impede the outflow of blood.Jumps in the female hormones estrogen and progesterone during the monthly cycle relax the venous wall.Contraceptive hormonal drugs can also have an effect - before taking them, it would be good to consult a phlebologist.
Lack of physical activity accelerates the development of varicose veins of the lower extremities.However, experts emphasize the significant role of the hereditary factor: if unattractive “stars” and “worms” from the vessels under the skin were observed in your parents, then with a high degree of probability both you and your children will one day personally encounter this problem.The tendency to varicose veins is transmitted through the female line - a gene is associated with the sex X chromosome, which can lead to weakness of the venous wall.
Among other things, varicose veins are more common in smokers, obese people, pregnant women and those who have other chronic diseases of the cardiovascular system.Professions whose representatives are predisposed to varicose veins of the legs are the following: surgeon, cashier, driver, programmer, flight attendant, loader, salesman, hairdresser, school teacher.
Pathogenesis
The veins of the lower extremities form a branched network, which consists of saphenous and deep veins, interconnected by perforating (communicant) veins.Through superficial veins, blood flows out from the subcutaneous tissue and skin, through deep veins - from other tissues.Communicating vessels serve to equalize the pressure between the deep and superficial veins.Blood normally flows through them only in one direction: from the superficial veins to the deep ones.
The muscle layer of the venous wall is weakly expressed and cannot force the blood to move upward.Blood flow from the periphery to the center is carried out due to residual arterial pressure and the pressure of the tendons located next to the vessels.The most important role is played by the so-called muscle pump.During physical activity, the muscles contract and the blood is squeezed upward because the downward movement is prevented by the venous valves.Maintaining normal blood circulation and constant venous pressure is influenced by venous tone.The pressure in the veins is regulated by the vasomotor center located in the brain.
Valve insufficiency and weakness of the vascular wall lead to the fact that blood, under the influence of a muscle pump, begins to flow not only up, but also down, putting excess pressure on the walls of blood vessels, leading to dilation of the veins, the formation of nodes and the progression of valvular insufficiency.
The blood flow through the communicating veins is disrupted.Reflux of blood from deep vessels to superficial vessels leads to a further increase in pressure in the superficial veins.Nerves located in the walls of the veins send signals to the vasomotor center, which gives the command to increase venous tone.The veins cannot cope with the increased load; they gradually expand, lengthen, and become tortuous.Increased pressure leads to atrophy of the muscle fibers of the venous wall and death of the nerves involved in the regulation of venous tone.
Classification
There are several classifications of varicose veins.This diversity is due to the polyetiology of the disease and the many variants of the course of varicose veins.
Stage-by-stage classification
Upon examination, pronounced varicose veins are visible on the legs.Patients complain of a feeling of fullness, paresthesia (“pins and needles”) in the lower legs, and night cramps.There is slight swelling of the feet, ankles and legs in the evenings.In the morning the swelling disappears.
Stage of decompensation.Dermatitis and eczema are added to the listed symptoms.Patients are bothered by itchy skin.The skin becomes dry, shiny, tightly fused with the subcutaneous tissue.Minor hemorrhages and subsequent deposition of hemosiderin cause hyperpigmentation.
Classification by shape
The following forms of varicose veins are distinguished:
- Segmental damage to subcutaneous and intradermal vessels without reflux.
- Segmental damage to veins with pathological discharge along the superficial or communicating veins.
- Widespread venous lesions with pathological discharge through the superficial or communicating veins.
- Widespread venous lesions with pathological discharge through the deep veins.
International classification
There is a recognized international classification of varicose veins, used by doctors in many countries around the world:
Class 0. There are no signs of varicose veins.Patients complain of heaviness in their legs.
Class 1. Networks of veins and spider veins (telangiectasia) are visually identified.Some patients experience muscle cramps at night.
Class 2. When examining the patient, dilated veins are visible.
Class 3. Swelling of the feet, ankles and legs appears, which does not disappear after a short rest.
Class 4. Upon examination, signs of lipodermatosclerosis are revealed (dermatitis, hyperpigmentation of the legs).
Class 5. Pre-ulcers form.
Class 6. Persistent trophic ulcers develop.
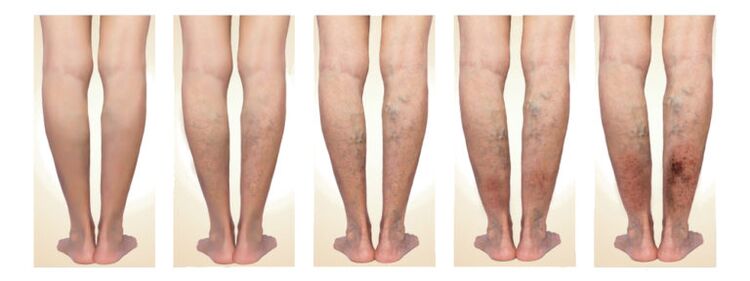
Symptoms and clinical manifestations
Varicose veins, which affect the veins of the lower extremities, are classified in international practice by stages, based on the neglect of the pathology and the severity of the manifestation.Each stage is diagnosed separately, all of them are characterized by different symptoms, based on which the treatment method is selected.
So, the symptoms that are a sign of varicose veins at different stages:
- At the first stage, the saphenous veins in the lower extremities have a barely noticeable pattern and protrude slightly above the skin, and slight redness is noticeable.There are complaints to the doctor about heaviness in the legs, evening swelling after a day of work.Swelling in the ankle area can be caused by excessively tight shoes, and cramps are also possible.It should be noted that often painful sensations can appear much earlier than visible signs.
- At the second stage, a typical appearance for diseased veins on the legs is already observed: they are significantly visible above the skin and can be felt with the fingers, looking like knots or beads.As it progresses, the saphenous vein of the lower limb becomes visible and takes on a tortuous shape of a dark blue or even black hue.
- At the third stage, varicose veins become more complicated, signs such as trophic changes in the veins in the legs are observed, the skin becomes dry and pale, daily swelling, and cramps.Symptoms often include a rash on the legs and itchy, itchy skin.
- Symptoms at the fourth, most severe stage are inflammatory processes in the saphenous veins of the lower limb, non-healing trophic ulcers, which are already difficult to treat.The key feature of this stage of disease is the addition of secondary infection and thrombophlebitis.With these manifestations, urgent hospitalization in a hospital and comprehensive use of treatment methods for the whole body are necessary.
Experts identify key risk factors:
- hereditary diseases associated with varicose veins in different parts of the body;
- hormonal disorders can increase blood clotting, decrease the elasticity of the veins in the legs;
- obesity, ascites, which increases the load on the legs, accompanied by dilation of the vein walls;
- pregnancy or lifting heavy objects increases pressure inside the abdominal cavity, which also contributes to weakening of the vascular walls and varicose veins;
- lack of stress on the legs, sedentary work are fraught with dilation of the veins in the legs;
- tight underwear, shoes of a smaller size, which pinches the vein, wearing heels, which causes stagnation of blood circulation in the veins in the legs;
- Varicose veins are often caused by kidney disease or cardiovascular disease, which causes swelling, observed in the dilation of the veins of the lower extremities.
Diagnostics
The main methods that involve the diagnosis of varicose veins of the legs are:
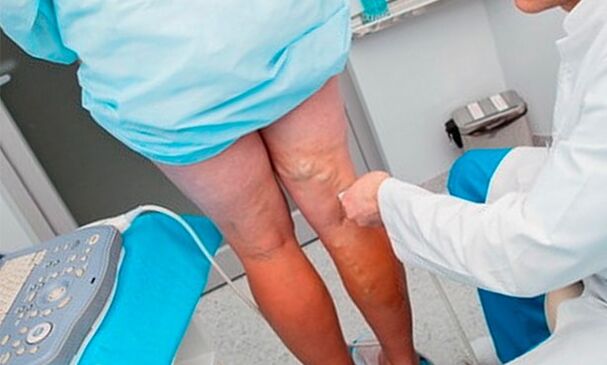
- An external examination of varicose veins in the legs should be performed by qualified doctors in a hospital.
- Doppler ultrasound to detect wall compactions in the veins of the lower extremities.Such diagnostics makes it possible to unambiguously determine the stage of the disorder.
- Duplex scanning of the veins in the legs, which is performed by a doctor at a specialized clinic, allows you to clearly identify varicose veins.This method, which combines ultrasound and Doppler examination, can check what is happening to the veins: the speed of blood circulation, the diameter of the leg veins, the functioning of the valves and the condition that characterizes varicose veins.
- A phleboscintigraphic study allows for high-precision analysis and, even at the initial stage, to learn about varicose veins in the legs and take timely preventive measures.It is carried out by introducing a special dye subcutaneously; such liquid in the vein is highlighted on the monitor in a contrasting color.
- Occlusion plethysmography.
- Using tomographic diagnostics of diseases (MRI, computed tomography) it is possible to identify complications accompanying varicose veins.
- Bandage or tourniquet tests for diagnosing diseases are used in combination as an additional method among various methods for determining the stage of varicose veins.
Deciphering the results of diagnosing varicose veins, as a rule, does not require much time.Most procedures take from 10 to 40 minutes, after which the attending physician will announce a diagnosis based on the information received.Diagnostics should be trusted only to an experienced clinic doctor who can make a clear and accurate diagnosis, because treatment at different stages involves different methods, treatment principles, and medications.
Features of treatment
Three main methods are used in the treatment of patients with varicose veins:
Conservative therapy
Conservative therapy includes general recommendations (normalization of motor activity, reduction of static load), physical therapy, use of elastic compression products (compression hosiery, elastic bandages), treatment with phlebotonics (diosmin + hesperidin, horse chestnut extract).
Conservative therapy cannot lead to a complete cure and restore already dilated veins.It is used as a prophylactic agent during preparation for surgery and when surgical treatment of varicose veins is impossible.
Compression sclerotherapy
With this treatment method, a special drug is injected into a dilated vein.The doctor injects elastic foam into the vein through a syringe, which fills the affected vessel and causes it to spasm.The patient is then put on a compression stocking to keep the vein in a collapsed state.After 3 days, the walls of the vein stick together.The patient wears the stocking for 1-1.5 months until dense adhesions form.
Indications for compression sclerotherapy are varicose veins, not complicated by reflux from deep vessels to superficial ones through communicating veins.In the presence of such pathological discharge, the effectiveness of compression sclerotherapy is sharply reduced.
Surgical treatment
The main treatment method for varicose veins complicated by reflux through the communicating veins is surgery.Many surgical techniques are used to treat varicose veins, including microsurgical techniques, radiofrequency and laser coagulation of the affected veins.
In the initial stage of varicose veins, photocoagulation or removal of spider veins with a laser is performed.In case of severe varicose veins, phlebectomy is indicated - removal of altered veins.Currently, this operation is increasingly performed using a less invasive technique - miniphlebectomy.
Prevention
Having discovered varicose veins, you need to take care of cleansing the body and normalizing blood circulation.To do this, first of all, they review the diet.The most useful for varicose veins are fresh products of plant origin:
- Vegetables - cabbage, tomatoes, sweet peppers, greens.
- Fruits - citrus fruits, apricots, apples, peaches, cherries, cherries, apples.
- Berries - strawberries, gooseberries, currants.
- There are many traditional medicine recipes based on fresh herbal ingredients.
Unfortunately, varicose veins are a chronic disease, and therefore “goes hand in hand” with a person throughout his life.Without prevention, the disease can lead to the development of more severe complications.
- It is not recommended to take too hot baths, or visit a sauna or stay in the sun for a long time in the heat.This leads to a decrease in venous tone, which certainly leads to congestion in the legs.
- Lead an active lifestyle, that is, move a lot.Thus, regular exercise will help not only strengthen blood vessels, but also improve the condition of the body as a whole.Moderate aerobics, swimming, cycling or running are ideal for preventing varicose veins.However, weightlifting and lifting things that are too heavy are contraindicated.
- Losing excess weight.People with a lot of body fat are more susceptible to this disease because they have more blood circulating in their body than a person of normal weight.This is why there is a heavy load on the vessels.In order for the pressure on the venous vessels to be less, obese people definitely need to get rid of extra pounds, as well as adhere to the right diet.As for the menu, it is advisable to minimize the consumption of too spicy foods.It is recommended to replace animal fats with vegetable oils.
- You should not wear very tight clothes, as well as socks or stockings with a tight elastic band, as they can put too much pressure on the veins, thereby impairing blood circulation.
- While sitting, you should not cross your legs, as during such a position, normal blood flow is also disrupted.
- Prolonged stay in a standing position has an extremely negative effect on the condition of the veins.If you have a standing job, try to move more often.Constant sitting is no less harmful.
- Nutrition should be normalized.Thus, regular constipation and intestinal dysbiosis can lead to the development of varicose veins.You should include in your menu foods rich in fiber, which helps improve intestinal motility, that is, digestion in general.
- Women should wear tight shoes and high-heeled shoes as little as possible.If you cannot refuse such shoes, then the heel should be no more than 3-4 centimeters in height.
- After heavy standing or sitting work, you should pour cold water over your legs, which will allow the veins to always be in good shape.Baths with the addition of pine salt are also useful.You can pour cold water on your feet in the morning.
- Prevention of varicose veins includes giving up bad habits, namely smoking, which has an extremely negative effect not only on the condition of the veins, but also on the entire human body.
- A light massage is considered an excellent preventive measure for this disease.This massage can be performed independently by stroking the skin of the lower extremities from bottom to top, and then in the opposite direction for 10 minutes.This self-massage is very useful in combination with massage procedures on the spine performed by a professional chiropractor or massage therapist.
- Prevention of venous dilatation also involves taking special medications that help maintain venous tone.
- Try to get rid of chronic fatigue and frequent stress.
- Doctors advise avoiding overheating and colds.
- If you have varicose veins, you should visit a phlebologist at least 2 times a year, who will monitor the condition of the veins and the stage of development of the disease.
To avoid illness, walk more, take a contrast shower, and visit the pool.Even if you don’t know how to swim, it’s useful to just stand in the water - the water column exerts a pressure of 60-70 mmHg on your legs.Art.This is enough to pump out blood stagnant in the veins.Gymnastics in the evenings has the same effect - while lying down, raise your legs and do the “bicycle” exercise.
In case of venous insufficiency, you need to use preventive knitwear (special tight stockings and tights create a kind of frame around the veins, preventing them from expanding).
By the way, such knitwear is very useful during pregnancy.Even in the first three months, when hormones are already having a negative effect.As the fetus grows, the density of the knitwear needs to be increased.During childbirth, it is also necessary, because this sharply increases blood pressure in the veins.
























